Low income, race, and rural residence among risk factors for low telemedicine literacy
Demographic factors including low income and living in a rural area are linked to low telemedicine literacy—which may limit access to plastic surgeons and other healthcare providers at a time of expanding use of telehealth and video visits, according to a report in the March issue of Plastic and Reconstructive Surgery.
“Our study finds that patients who fall into specific socioeconomically disadvantaged groups are at the highest risk of being underserved by telehealth services,” comments senior author Kavitha Ranganathan, MD, of Brigham and Women’s Hospital and Harvard Medical School. “The findings may help in targeting at-risk communities for interventions to increase telemedicine literacy and access.”
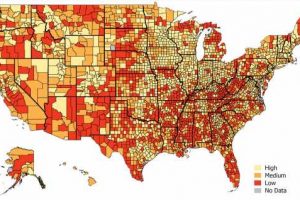
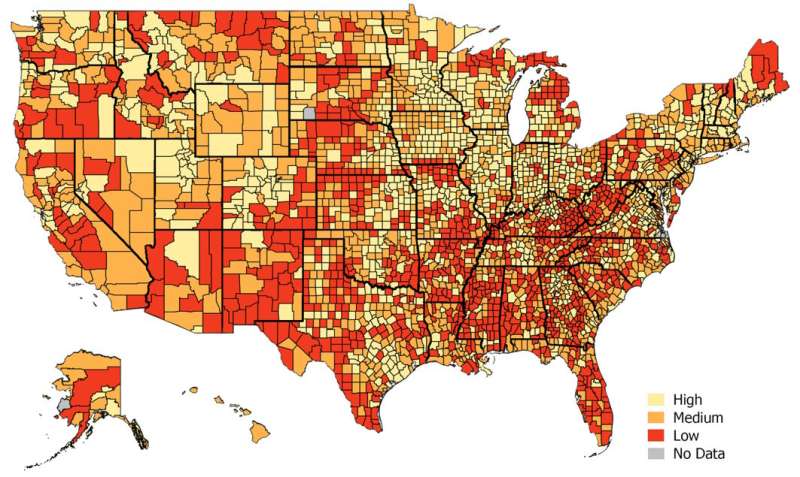
Does your county have a low ‘Technology Literacy Index’?
Use of telemedicine in the US healthcare system has increased dramatically since the start of the COVID-19 pandemic, facilitated by the 2020 CARES Act. “Due to its convenience, telemedicine will undoubtedly play an important role in plastic surgery practices moving forward,” says Dr. Ranganathan. “However, barriers to successful telemedicine visits may exacerbate existing health disparities among disadvantaged groups.”
The researchers identified sociodemographic and geographic factors associated with barriers to successful telemedicine visits, based on a 2019 Pew Research Institute survey on internet and technology use. Using the survey data, the researchers developed a new Technology Literacy Index (TLI), consisting of three factors: access to the internet, access to a smartphone, and comfort with technology.
The TLI and factors associated with barriers to telemedicine were then extrapolated to the population using 2018 US Census data. This allowed the researchers to classify telemedicine literacy as high, medium, or low for more than 3,000 counties, parishes, and boroughs nationwide.
A wide range of factors were associated with a low TLI, indicating low telemedicine literacy. Independent risk factors (in descending order of importance) included widowed marital status, less than high-school education, age over 65, disabled employment status, some college but no degree, and Black people or African American race. Higher income and higher education were associated with a higher TLI.
Extrapolated to the county level, the data showed varying levels of telemedicine literacy across the United States. Counties with low TLI had a lower median annual income, $44,000 versus $60,000; and a lower percentage of the population with a college degree, 17% versus 26%.
Policy implications for improving telemedicine literacy
Rural areas were three times more likely to be classified with low TLI. Areas with the highest proportions of Black people or African American residents were also more likely to have low telemedicine literacy: 78%, compared to 49% of areas with the lowest proportions of Black residents.
“[T]he largest barriers to wider adoption are social, with one of them being inadequate digital literacy,” the researchers write. Previous studies have linked many of the same factors to lower digital literacy, and to decreased physician visits since the start of the COVID-19 pandemic.
“Within the field of plastic surgery, these disparities highlight specific at-risk populations,” Dr. Ranganathan and co-authors add. For example, some subgroups of reconstructive surgery patients may have sociodemographic risk factors for telemedicine-related health disparities.
“Insurers, policymakers, healthcare providers, and patient champions may be able to target specific communities for interventions to increase telemedicine literacy and access,” Dr. Ranganathan and co-authors conclude. “As plastic surgery and healthcare more broadly is becoming increasingly dependent on the ability to utilize technology, appropriate efforts to mitigate and prevent adding to pre-existing healthcare disparities are critical.”
More information:
Andrew Harris et al, Disparities in Telemedicine Literacy and Access in the United States, Plastic & Reconstructive Surgery (2023). DOI: 10.1097/PRS.0000000000009939
Journal information:
Plastic and Reconstructive Surgery
Source: Read Full Article